In this prospective study, we evaluated the trajectory of QoL and its specific domains in patients with hematological malignancies during their hospitalization for auto- and allo-HSCT. Our results showed that overall QoL and its domains changed significantly during hospitalization, except for Social/Family Well-Being. The changes in the QoL domains were parabolic, deteriorating between admission to the hospital and the sixth day after transplantation, then improving at discharge, but not reaching baseline levels. It is noteworthy that the trajectory of the Emotional Well-Being QoL has a different trend than the other subscales: constant up to the sixth day after HSCT, and improving on discharge from the hospital. Moreover, we found no difference in QoL trajectory between patients hospitalized for auto-HSCT and those hospitalized for allo-HSCT.
The trajectory of changes in general QoL revealed in our study is partially in line with results from other studies (see6,20). On the one hand, our research aligns with previous research showing a drastic deterioration of QoL, occurring rapidly, within one week of hospitalization17,18,20. Nevertheless, in those studies, the decline of QoL persisted at the time of discharge, which is inconsistent with our results. It should be noted that those studies included fewer time points than ours. In the Ozturk et al.21 study, no changes were observed in the overall QoL of patients hospitalized for HSCT. However, that study included only two measurement points (at the beginning and end of hospitalization) and was conducted on a small study group. Although there are many studies on the QoL of transplanted patients, most consider the period of hospitalization as a single time when measuring QoL12,16. Our findings support the need to assess QoL several times during hospitalization for HSCT, which can help organize psychological and medical care during these types of hospitalizations.
In our study, similar changes in QoL were observed in the following dimensions: Physical (PWB-QoL, measured symptoms: pain, energy level, side effects, nausea); Functional (FWB-QoL, measured symptoms: sense of fulfillment in life and work); and connected with Bone Marrow Transplant itself (BMTS, measured symptoms: worries about the transplant and being able to cope with it). These scales focus on physical symptoms and psycho-physical functioning related to HSCT. Therefore, most likely, the general QoL of transplanted patients during hospitalization is most influenced by aspects connected with physical symptoms, and factors associated with the psycho-physical state during HSCT. On the other hand, emotional and social/family well-being impacts transplant patients’ QoL to a lesser extent than other dimensions. The trend of changes observed in Emotional Well-Being (consistently lower over the first three measurement points, and increasing significantly on the day of discharge) indicates that although patients’ moods were lower during the entire HSCT hospitalization than on the day of discharge from the hospital, they were stable during treatment. It is worth noting that patients’ moods did not decline even during periods of worse physical well-being. In our studies, HSCT treatment did not influence changes in social/family well-being assessment during treatment, which may indicate a stable bond with family and friends during hospitalization for HSCT. Meanwhile, the study by Ozturk et al.21 showed increased scores in social/family dimension. Our results, and those of Ozturk et al.21, contradict the generally accepted view of the threat to social bonds from long-term illness and hospitalization. These conflicting results require further analysis.
What may be surprising for all dimensions of QoL is that the level and trajectory of changes in QoL were not influenced by the type of treatment (auto-HSCT or allo-HSCT). We expected significant differences here, taking into account our own clinical experience and previous research findings. The literature provides conflicting data regarding differences in QoL in patients treated with auto- vs. allo-HSCT. Some researchers point to similar impairment in QoL for both types of HSCT17,18, and others show worse QoL in patients transplanted from allogeneic donors22,23. Possible and specific complications related to allo-HSCT and prolonged hospitalization in this type of HSCT may justify treating auto- and allo-HSCT separately when assessing a patient’s QoL. Moreover, Morishita et al.24 emphasize that QoL and other outcomes of psychological status should be evaluated independently, even in the specific type of HSCT from a haploidentical donor. At the same time, some researchers indicate similar QoL parameters for haploidentical patients10. In this context, our research indicating a lack of differences in all QoL dimensions between patients hospitalized for auto- and allo-HSCT is surprising and adds new knowledge to this discussion. However, it is difficult to explain this result, taking into account such risk factors in the allo-HSCT group as prolonged hospitalization with isolation, more lines of prior therapy, more frequent use of radiotherapy in the conditioning regimens, and diagnosis of acute leukemia. One possible explanation for non-inferior QoL in the allo-HSCT group may be more careful attention given by medical staff to patients in this group. Further studies in this area are indicated.
As our results indicate, it is not the specific type of HSCT that affects the quality of life of patients. This observation leads us to wonder whether the quality of life is not influenced to a greater extent by the prolonged hospital stay, isolation, and the patient’s thoughts and emotions related to undergoing a major medical procedure. Such a conclusion would allow us to generalize our results to other groups of patients undergoing long hospitalizations due to the need for burdensome medical procedures (e.g., some surgeries and other transplant procedures). Comparative studies would be necessary to assess whether the impact of long hospitalizations on quality of life is similar across different patient groups. HSCT is a specific procedure, and the lack of differences in patient outcomes may be due to the type of HSCT itself or, as other studies suggest, may emerge over time.When comparing the results of our study with others, the initial level of QoL in patients at the beginning of HSCT hospitalization is also noteworthy. In other studies, this level is significantly lower especially in allo-HSCT patients17. Perhaps a critical assessment of the current research on QoL results should be carried out, considering the broader aspects of including patients in studies, such as age, initial health status, diagnosis, quality of previous treatment, and so on. Without this knowledge, simple references to other results will be error-prone and may lead to inappropriate conclusions.
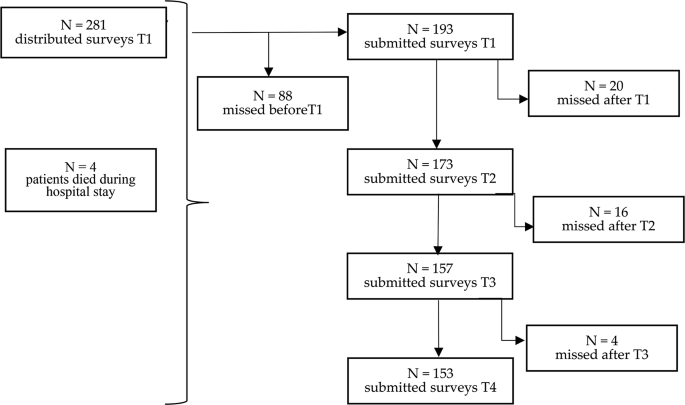
This study has some limitations. First, we employed a relatively small sample of patients from a single transplantation center. Furthermore, the study population was somewhat homogeneous in terms of socio-demographic factors, and it is essential to exercise caution when extrapolating these results to the more diverse population of transplanted patients. As a result, the findings might not apply to patients in other regions/transplantation centers who use different supportive care methods during the HSCT procedure. To understand the trajectory of QoL changes over the recovery period, expanding the evaluation by additional time points is imperative. Another limitation of our study is that a specific group of people was lost, especially between the T1 and T2 measurements. Since the motives of these patients were not controlled (also for ethical reasons), the conclusions may be biased because our group could have overrepresented more motivated patients or those in better physical condition.
In conclusion, the quality of life in patients hospitalized for HSCT changes dramatically. Changes in the QoL trajectory are parabolic in nature, reaching their nadir a few days after HSCT, regardless of the type of HSCT (auto vs. allo). Therefore, medical and psychological support during the entire hospitalization period should be equally intensive for patients undergoing both types of HSCT. Our findings highlight the need to monitor patients’ quality of life during the entire hospitalization period and to implement adequate and individualized supportive care interventions to improve the patient experience when undergoing HSCT. However, further prospective studies on larger groups of transplanted patients, preferably with additional studied time points, are needed.