Baseline characteristics
Baseline characteristics of the four groups are shown in Table 1. The active minimization and minimization groups were older than the other two groups. The most common underlying liver disease for HCC was hepatitis B in all groups, but there were significant differences. Pretransplant model for end-stage liver disease (MELD) scores were significantly different between the four groups, with minimal differences in median values. Living donors showed a >75% advantage in all groups. Donor age, sex, and graft steatosis were similar between groups. Median AFP values for the conventional, aggressive minimization, minimization, and high exposure groups were 6.5, 8.0, 5.6, and 11.0 ng/mL, respectively (P = 0.009). PIVKA II at LT was 31.5, 113.5, 38.0, and 28.0 mAU/mL, respectively (P < 0.001), with significant differences between groups, with higher values in the aggressive minimization group. Type of bridging therapy differed significantly between groups, with higher incidence of systemic therapy or radiotherapy in the aggressive minimization and minimization groups (11.9%, 37.5%, 17.4%, 5.9%, respectively, P< 0.001). Regarding explant pathology, most variables were similar between groups, except for poor differentiation and satellite nodules. The four groups had similar HCC risk categories according to the Milan criteria and French risk score.
immunosuppressant
Among the entire study population, TAC was initiated before at least 4 days postoperatively. Interleukin-2 receptor antibody was used for induction therapy in almost all patients except one, with a total dose of 40 mg used in his 99.0% of recipients. After his 3 months of LT, 33.3% of patients were taking their MMF and 31.8% were taking their mTOR inhibitors (Figure S1).
Median tacrolimus trough levels were well stratified by CET group throughout the study period (Figure 2). Parameters related to intrapatient variation showed significant differences between groups. Notably, a higher coefficient of variation was observed in the aggressive minimization group than in the other groups (Table S1). Immunosuppressant regimens also differed between groups. The proportion of TAC monotherapy was highest in the high exposure group (31.0%, 12.5%, 26.9%, 68.0%, respectively), and the proportion of TAC + mTORi showed an opposite trend depending on the degree of CET (22.7%, 81.2%). %, 48.4% and 2.0% respectively). Oral steroids were maintained similarly in most patients in the four groups.
HCC recurrence and death
During a mean follow-up period of 43.2±20.2 months, 74 (14.5%) patients experienced HCC recurrence and 77 (15.0%) patients died. Median time from LT to HCC recurrence was 13.4 (IQR 9.4–23.1) months (Figure S2). Using Kaplan-Meier analysis, 5-year recurrence-free survival was not significantly different between the four CET groups (84.0 for the conventional, aggressive minimization, minimization, and high exposure groups) %, 74.2%, 84.5%, and 84.2%, respectively, P = 0.671; Figure 3a). In contrast, 5-year overall survival differed significantly between groups, with active minimization and high exposure groups showing lower survival than other groups (85.6%, 70.5%, respectively) 85.2%, 76.2%, P = 0.004, Fig. 3b). The distribution of causes of death is shown in Figure S3, and there are no statistically significant differences.
Kaplan-Meier analysis of survival outcomes. (be) HCC recurrence = free survival, (b) Overall survival.
In univariate and multivariate Cox analyzes (Table 2), CET group was not a significant risk factor for HCC recurrence (HR 1.13 for aggressive minimization, P = 0.790; HR 0.99 for minimization, P = 0.973; HR 0.94 for minimization (high exposure vs. conventional exposure); P = 0.848). Other important risk factors for HCC recurrence were age (HR 0.95, P = 0.004), BMI (HR 0.92, P = 0.033), pre-transplant MELD score (HR 0.94, P = 0.017), log AFP (HR 1.18, P = 0.033). 0.018), bridging therapy (HR 0.21, P = 0.001 for none, HR 2.38, P = 0.003 for systemic or radiotherapy plus locoregional therapy), number of viable tumors (HR 1.07, P = 0.006), max. tumor size (HR 1.13, P = 0.044), microvascular invasion (HR 2.14, P = 0.005), and acute rejection within 3 months (HR 2.10, P = 0.006).
In contrast, aggressive minimization was a significant risk factor for overall mortality in multivariate analysis when compared with the conventional group (HR 5.19, P = 0.001). Minimization had no effect on overall mortality (HR 1.16, P = 0.640), and the high exposure group showed marginal risk (HR 1.64, P = 0.091) compared to the conventional group. Other mortality risk factors were BMI (HR 0.91, P = 0.012), deceased donor (HR 2.00, P = 0.008), log AFP (HR 1.18, P = 0.007), systemic therapy or radiotherapy and locoregional therapy ( HR 3.71, P < 0.001), number of viable tumors (HR 1.06, P = 0.006), satellite nodules (HR 4.52, P < 0.001), and mTORi use within 3 months (HR 0.25, P < 0.001) .
Matched and subgroup analyzes for HCC recurrence
We performed a matching analysis for HCC recurrence between the conventional CET group and three other CET groups. Baseline characteristics were balanced between matched groups (Tables S2–S4). The results also revealed that there was no significant relationship between CET group and HCC recurrence (Figure S4). We also performed subgroup analyzes stratified by HCC recurrence risk, including within/above Milan criteria, French risk score 2/>2, presence or absence of systemic therapy or radiotherapy before LT, and presence or absence of mTORi (Figure 4 ). However, no significant differences were observed between his CET groups in these subgroups.
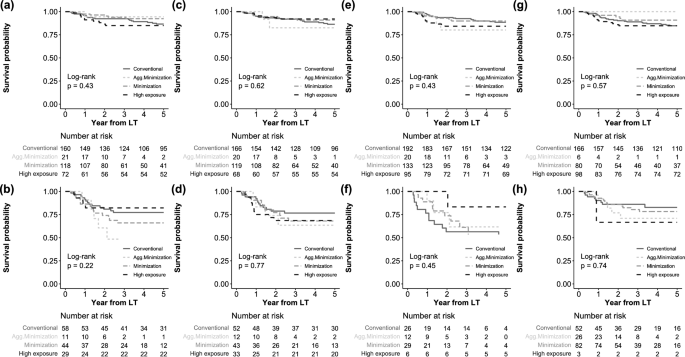
Subgroup analysis of HCC recurrence. (be) In Milan, (b) over Milan, (c) French risk score ≤ 2, (d) French risk score > 2, (e) Without systemic therapy or radiation therapy, (f) When combined with systemic therapy or radiation therapy, (g) without mTORi, and (h) using mTORi.

